Measles Outbreak: 7 US States Report Cases in April 2026
Seven U.S. states have confirmed measles cases in April 2026, prompting a public health alert due to the highly contagious nature of the virus and the importance of vaccination to prevent further spread.
As April 2026 unfolds, a significant public health concern has emerged across the nation: a new measles outbreak US 2026. This highly contagious viral disease, once nearly eradicated thanks to widespread vaccination efforts, is now making an unwelcome return, with confirmed cases reported in no fewer than seven U.S. states. Understanding the implications of this development is crucial for every citizen, as the virus poses a serious threat, especially to unvaccinated individuals and vulnerable populations.
Understanding the Current Measles Outbreak
The current measles outbreak in the U.S. in April 2026 represents a critical moment for public health. Measles, caused by a virus in the paramyxovirus family, is known for its extreme contagiousness, capable of spreading through the air via respiratory droplets from coughing or sneezing. This section delves into the specifics of the current situation, outlining the affected states and the initial assessments of the outbreak’s scope.
Affected States and Initial Reports
As of April 2026, health authorities have confirmed measles cases in seven distinct U.S. states. These states, spread across different regions, indicate a broader, albeit localized, resurgence of the disease. Initial reports suggest varied origins for these cases, ranging from international travel-related exposures to community-level transmission among unvaccinated populations.
- California: Several cases identified, primarily linked to international travelers.
- Texas: Clusters observed in areas with lower vaccination rates.
- New York: Isolated cases reported, prompting increased vigilance in urban centers.
- Florida: Cases detected in both children and adults, emphasizing broader susceptibility.
- Illinois: Public health officials are tracing contacts to prevent further spread.
- Arizona: A small number of cases, but a concern due to tourist traffic.
- Washington: Cases identified, leading to enhanced monitoring in schools.
The rapid identification and reporting of these cases are vital for implementing timely public health interventions. Early detection allows for immediate contact tracing and isolation measures, which are essential in containing the spread of such a virulent disease. The diverse geographical spread underscores the need for a unified and robust national response to this emerging health challenge.
The initial assessments by the Centers for Disease Control and Prevention (CDC) and state health departments highlight the urgency of the situation. They are working collaboratively to understand the genetic sequencing of the circulating virus strains, which can provide insights into their origins and potential pathways of transmission. This scientific approach is foundational to developing effective containment strategies.
Understanding the current measles outbreak requires a clear picture of where and how the virus is manifesting. The involvement of multiple states signals that this is not an isolated incident but a pattern that demands immediate and comprehensive attention from both health officials and the general public. The information gathered from these initial reports is crucial for guiding subsequent actions.
The Resurgence of Measles: Why Now?
Measles was declared eliminated in the U.S. in 2000, a monumental achievement attributed to the highly effective measles, mumps, and rubella (MMR) vaccine. The current resurgence, marked by the measles outbreak US 2026, raises critical questions about the factors contributing to its return. This section explores the underlying reasons behind this concerning trend, focusing on vaccination rates and global travel.
Declining Vaccination Rates
One of the primary drivers behind the re-emergence of measles is the decline in vaccination rates in certain communities. The concept of ‘herd immunity’ relies on a high percentage of the population being vaccinated to protect those who cannot be, such as infants or individuals with compromised immune systems. When vaccination rates drop below the critical threshold (typically around 95% for measles), the virus finds fertile ground to spread.
- Misinformation: The spread of false information about vaccine safety has led some parents to delay or refuse vaccinations for their children.
- Vaccine hesitancy: A growing skepticism towards conventional medicine and public health recommendations.
- Accessibility issues: In some underserved areas, access to vaccination services may be limited.
The impact of declining vaccination rates is profound, creating pockets of susceptibility where the measles virus can rapidly gain traction. These vulnerable communities act as incubators for the disease, allowing it to spread more easily and potentially leading to larger outbreaks. Addressing vaccine hesitancy through accurate information and accessible services is paramount.
Impact of Global Travel
In an interconnected world, global travel plays a significant role in the spread of infectious diseases. Measles cases often originate from individuals contracting the virus abroad and then bringing it back into the U.S. where they can infect unvaccinated contacts. The ease and frequency of international travel mean that a single case can quickly become a localized outbreak if community immunity is insufficient.
Travelers to regions with ongoing measles outbreaks are particularly at risk. Upon returning, if they are unvaccinated and become infected, they can unknowingly expose others in their communities. This scenario underscores the importance of pre-travel vaccination and awareness, not only for personal protection but also for safeguarding public health.
The interplay between declining vaccination rates and global travel creates a perfect storm for measles resurgence. While individual choices regarding vaccination are personal, their collective impact has significant public health consequences. Understanding these dynamics is crucial for developing effective strategies to prevent future outbreaks and protect community health.
Recognizing Measles Symptoms and Complications
Early recognition of measles symptoms is vital for prompt diagnosis, isolation, and prevention of further transmission, especially in the context of the current measles outbreak US 2026. This section details the characteristic signs of measles and outlines the potential complications, emphasizing why this seemingly childhood illness can be very serious.
Typical Symptoms and Progression
Measles typically begins with a prodromal phase characterized by a constellation of non-specific symptoms, making early diagnosis challenging. This phase usually lasts for 2-4 days before the more distinctive rash appears. Patients are contagious even during this early stage, often before they realize they have measles.
- Fever: Often high, reaching 104°F (40°C) or more.
- Cough: A dry, persistent cough.
- Runny nose: Similar to a common cold.
- Conjunctivitis: Red, watery eyes.
- Koplik’s spots: Small, white spots with bluish-white centers on a red background found inside the mouth, usually appearing 1-2 days before the rash. These are pathognomonic for measles.
Following the prodromal phase, the characteristic measles rash erupts. The rash typically starts on the face, behind the ears, and along the hairline, then spreads downwards to the neck, trunk, arms, and legs. The rash consists of red, flat spots that can be slightly raised and often merge, giving it a blotchy appearance. The rash usually lasts for about 5-6 days before fading, generally in the same order it appeared.
During the entire course of the illness, individuals with measles are highly contagious. They are considered infectious from four days before the rash appears to four days after the rash starts. This extended period of contagiousness, coupled with the virus’s airborne transmission, makes containment particularly challenging if not identified early.
Serious Complications of Measles
While often viewed as a benign childhood disease, measles can lead to severe and life-threatening complications, especially in young children, pregnant women, and individuals with weakened immune systems. These complications underscore the importance of vaccination as the best protective measure.
- Ear infections: Common bacterial infections that can lead to permanent hearing loss.
- Diarrhea and vomiting: Can cause severe dehydration, particularly in young children.
- Pneumonia: A common and serious complication, especially in infants, and a leading cause of measles-related deaths.
- Encephalitis: Inflammation of the brain, occurring in about 1 in 1,000 cases, which can lead to convulsions, deafness, or intellectual disability.
- Subacute sclerosing panencephalitis (SSPE): A rare but fatal degenerative neurological disease that can develop years after measles infection, even if the individual appears to have fully recovered.
These complications highlight that measles is far more than just a rash and fever. Its potential for severe health outcomes, including permanent disability and death, makes the current outbreak a serious public health concern. Recognizing these symptoms and understanding the risks are crucial steps for individuals and healthcare providers alike.
Public Health Response and Containment Strategies
In response to the measles outbreak US 2026, public health authorities at both federal and state levels have rapidly initiated comprehensive containment strategies. These efforts are multi-faceted, aiming to limit the spread of the virus, protect vulnerable populations, and provide accurate information to the public. Effective coordination and swift action are paramount in managing such a highly transmissible disease.
Enhanced Surveillance and Contact Tracing
A cornerstone of any outbreak response is robust surveillance and meticulous contact tracing. Public health departments in the affected states are intensifying their efforts to identify new cases, track their contacts, and ensure appropriate isolation measures are in place. This involves:
- Active case finding: Healthcare providers are urged to report any suspected measles cases immediately to local health authorities.
- Laboratory confirmation: All suspected cases undergo laboratory testing to confirm measles infection.
- Contact identification: Public health teams interview confirmed cases to identify anyone they may have exposed during their infectious period.
- Monitoring and quarantine: Contacts are monitored for symptoms and, if unvaccinated, may be advised to self-quarantine to prevent potential further spread.
This proactive approach helps to break chains of transmission and prevent the virus from establishing deeper roots within communities. The speed and thoroughness of these processes are critical to successful containment, especially given measles’ high infectivity rate. Timely communication between state health departments and the CDC ensures a unified national picture of the outbreak.
Community Outreach and Vaccination Drives
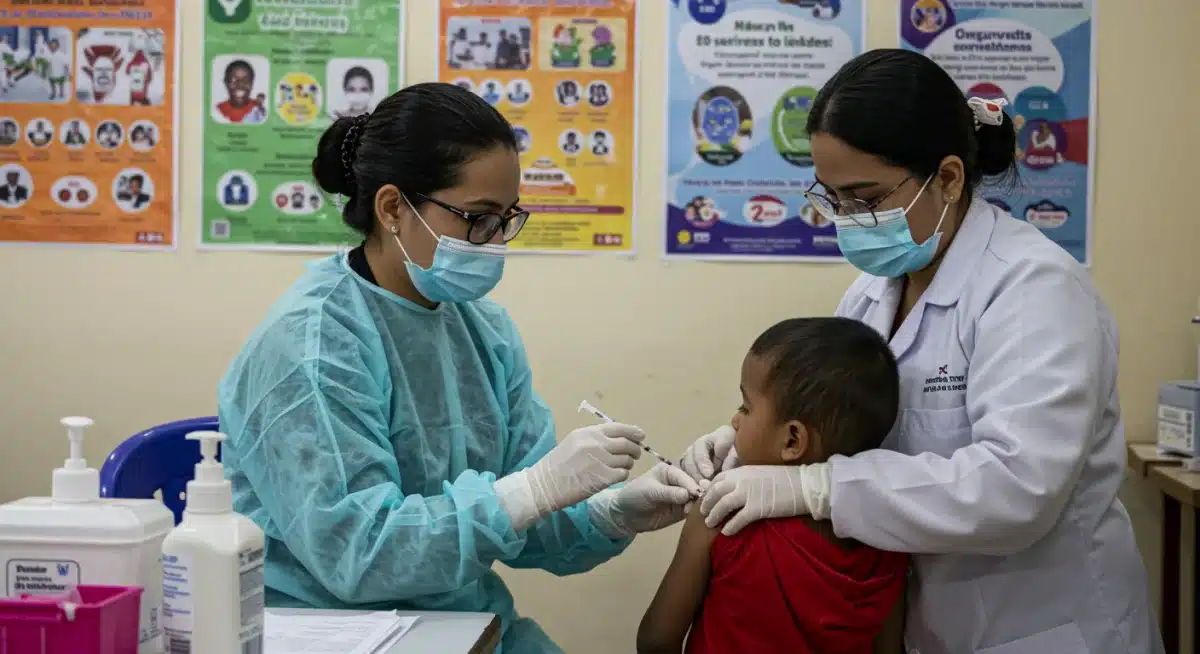
Beyond surveillance, public health agencies are focusing heavily on community outreach and accelerating vaccination drives. Education campaigns are being launched to inform the public about the risks of measles, the symptoms to watch for, and the importance of vaccination. These campaigns often target communities identified with lower vaccination rates.
Vaccination clinics are being established in accessible locations, offering the MMR vaccine to eligible individuals. Special attention is given to ensuring that children receive their routine vaccinations on schedule and that adults who are unsure of their immunity status can get tested or receive booster shots. These efforts are designed to bolster herd immunity and create a protective barrier against the virus.
Public health messaging also emphasizes the importance of good hygiene practices, such as frequent handwashing and covering coughs and sneezes, although vaccination remains the most effective preventive measure against measles. The goal is to empower individuals with the knowledge and tools to protect themselves and their communities from this preventable disease.
The collective response from public health agencies is a testament to the dedication to safeguarding community health. By combining rigorous surveillance with proactive vaccination and education initiatives, authorities aim to swiftly bring the current measles outbreak under control and prevent future recurrences.
The Critical Role of Vaccination in Prevention
Vaccination remains the single most effective tool in preventing measles and controlling outbreaks like the current measles outbreak US 2026. The MMR vaccine has a proven track record of safety and efficacy, providing robust protection against measles, mumps, and rubella. Understanding its importance is crucial for public health.
Efficacy and Safety of the MMR Vaccine
The MMR vaccine is a live, attenuated (weakened) virus vaccine that stimulates a strong immune response without causing the disease. It is typically administered in two doses:
- First dose: Given between 12 and 15 months of age.
- Second dose: Given between 4 and 6 years of age.
With two doses, the MMR vaccine is about 97% effective at preventing measles. A single dose is about 93% effective. This high efficacy rate is what allowed the U.S. to achieve measles elimination previously. Extensive scientific research and decades of use have consistently demonstrated the vaccine’s safety profile, with severe adverse reactions being extremely rare.
Common side effects are generally mild and temporary, such as fever or a mild rash. The benefits of vaccination far outweigh the minimal risks, especially when considering the potential severity of measles complications. Public health organizations worldwide endorse the MMR vaccine as a critical component of childhood immunization schedules.
Addressing Vaccine Misinformation
One of the persistent challenges to maintaining high vaccination rates is the spread of misinformation and disinformation about vaccine safety. Baseless claims, often circulated online, can create vaccine hesitancy and lead individuals to forego this essential protection. Public health efforts are actively working to counteract these narratives by:
- Providing accurate and evidence-based information from trusted sources like the CDC and WHO.
- Engaging with communities to address concerns and answer questions about vaccines.
- Highlighting the real-world impact of measles outbreaks in unvaccinated populations.
Combating misinformation is a continuous battle, but it is essential for protecting public health. Healthcare providers play a crucial role in counseling patients and parents, offering clear, factual information, and building trust. The message is clear: vaccination is a safe and effective way to protect against measles.
The role of vaccination cannot be overstated. It is not only about individual protection but also about community protection through herd immunity. Maintaining high vaccination coverage is the best defense against measles outbreaks and ensures that vulnerable individuals are also safeguarded from this dangerous disease.
Personal and Community Actions to Mitigate Risk
In light of the measles outbreak US 2026, both individuals and communities have a crucial role to play in mitigating the risk of further spread. Beyond public health interventions, personal responsibility and collective action are vital to protecting health. This section outlines practical steps everyone can take to contribute to containment efforts.
Ensuring Your Vaccination Status
The most important step an individual can take is to verify their vaccination status. If you or your family members are unsure whether you have received two doses of the MMR vaccine, consult with your healthcare provider. They can check your vaccination records or, if records are unavailable, administer the vaccine. This is particularly important for:
- Travelers: Especially those planning international trips to areas with ongoing measles activity.
- Healthcare workers: Due to their increased exposure risk to infectious diseases.
- Students: Living in close quarters can facilitate rapid transmission.
- Anyone born after 1957: Who may not have natural immunity from prior infection.
If you are unvaccinated or under-vaccinated, getting the MMR vaccine is a straightforward and highly effective way to protect yourself and those around you. It’s a simple yet powerful act of public health responsibility.
Practicing Good Hygiene and Isolation
While vaccination is paramount, general hygiene practices also play a supporting role in reducing the spread of respiratory viruses. These habits become even more critical during an outbreak:
- Handwashing: Frequent and thorough handwashing with soap and water.
- Respiratory etiquette: Covering coughs and sneezes with a tissue or your elbow.
- Avoiding touching face: Keeping hands away from eyes, nose, and mouth.
Crucially, if you or a family member develop symptoms consistent with measles, it is imperative to isolate yourselves and contact your healthcare provider immediately. Call ahead before visiting a clinic or emergency room to allow staff to take precautions to prevent further transmission. Early isolation is key to breaking the chain of infection and protecting the wider community.
Community actions also involve supporting public health initiatives, such as participating in vaccination drives and sharing accurate information within social circles. By working together, individuals and communities can significantly reduce the impact of the current measles outbreak and safeguard public health for everyone.
Looking Ahead: Long-Term Implications and Future Preparedness
The measles outbreak US 2026 serves as a stark reminder of the ongoing challenges in public health and the necessity of sustained vigilance. This section explores the potential long-term implications of such outbreaks and discusses strategies for future preparedness, ensuring that the U.S. remains resilient against vaccine-preventable diseases.
Strengthening Public Health Infrastructure
The current outbreak highlights the need for continuous investment in and strengthening of public health infrastructure. This includes robust surveillance systems, well-funded state and local health departments, and a highly trained public health workforce. A strong infrastructure allows for rapid detection, investigation, and response to infectious disease threats.
- Enhanced laboratory capacity: To quickly diagnose and characterize circulating pathogens.
- Improved data sharing: Seamless exchange of information between federal, state, and local agencies.
- Sufficient staffing: Ensuring enough epidemiologists, contact tracers, and public health nurses.
Without adequate resources, public health agencies struggle to keep pace with evolving threats, making communities more vulnerable to outbreaks. Investing in these areas is not just a response to a crisis but a proactive measure for long-term health security.
Sustaining High Vaccination Coverage
The most critical long-term strategy is to maintain and, where necessary, increase vaccination coverage rates across all demographics. This requires ongoing public education campaigns, accessible vaccination services, and policies that support immunization. Efforts must be made to:
- Counter vaccine misinformation: Through consistent, evidence-based communication.
- Address disparities: Ensuring equitable access to vaccines for all communities.
- Promote routine immunization: Emphasizing the importance of adhering to recommended vaccination schedules.
Achieving and sustaining herd immunity is a collective responsibility that requires continuous effort from healthcare providers, public health officials, educators, and community leaders. It protects not only individuals but also the most vulnerable members of society. Future preparedness hinges on a well-immunized population.
The long-term implications of measles outbreaks extend beyond immediate illness, potentially impacting healthcare costs, school attendance, and even economic productivity. By learning from the current situation and proactively implementing comprehensive preparedness strategies, the U.S. can better safeguard its population against future health crises and ensure that vaccine-preventable diseases remain a relic of the past.
| Key Aspect | Brief Description |
|---|---|
| Outbreak Scope | Measles cases confirmed in 7 U.S. states as of April 2026, indicating regional spread. |
| Primary Causes | Declining vaccination rates and global travel contributing to resurgence. |
| Prevention Key | MMR vaccine is highly effective and safe; essential for individual and herd immunity. |
| Public Response | Enhanced surveillance, contact tracing, and community vaccination drives are underway. |
Frequently Asked Questions About the Measles Outbreak
As of April 2026, confirmed measles cases have been reported in seven U.S. states: California, Texas, New York, Florida, Illinois, Arizona, and Washington. Public health officials are actively monitoring the situation in these areas to prevent further spread and protect communities.
Measles typically begins with a high fever, cough, runny nose, and red, watery eyes. These are followed by the appearance of Koplik’s spots inside the mouth, and then a characteristic red, blotchy rash that starts on the face and spreads downwards.
The MMR vaccine is highly effective. With two doses, it provides approximately 97% protection against measles. A single dose offers about 93% protection. This vaccine is considered safe and is a critical tool in preventing outbreaks and protecting public health.
If you suspect you have measles, isolate yourself immediately to prevent exposing others. Contact your healthcare provider by phone before visiting a clinic or emergency room, so they can take appropriate precautions. Early diagnosis and isolation are crucial for containment.
The re-emergence of measles is primarily attributed to declining vaccination rates in certain communities, leading to insufficient herd immunity. Additionally, international travel from regions with ongoing outbreaks can introduce the virus, which then spreads among unvaccinated populations.
Conclusion
The measles outbreak US 2026 serves as a powerful reminder of the fragility of public health achievements and the critical importance of sustained vigilance. While measles was once considered eliminated in the United States, its resurgence underscores the ongoing challenges posed by declining vaccination rates and global interconnectedness. The coordinated efforts of public health agencies, coupled with individual responsibility in ensuring vaccination status and practicing good hygiene, are paramount in containing this current outbreak. Moving forward, continued investment in robust public health infrastructure, alongside persistent efforts to counter misinformation and promote routine immunization, will be essential to safeguard communities and ensure that vaccine-preventable diseases like measles remain under control for generations to come. Protecting public health is a collective endeavor, requiring active participation from every member of society.